Is Pancreas Cancer a Battle You Can Win? Discover the answer in this guide.
One common question that echoes in the minds of patients and their loved ones is, “Is pancreas cancer treatable?”
Pancreatic cancer is a challenging adversary, raising numerous concerns and questions for those affected.
Let’s explore the latest advancements and support available to decode the answer to this question about pancreatic cancer treatment.
What is Pancreatic Cancer?

Pancreatic cancer happens when cells in your pancreas change and grow too quickly, creating growth.
This growth is when cells in the pancreas start multiplying uncontrollably, forming a cancerous tumor.
The pancreas is a gland in the middle part of the body, between your back and stomach. It makes enzymes to help digest food. It also makes hormones (endocrine) control the amount of sugar in the blood.
Most types of pancreatic cancer begin in the tubes of the organ. The major pancreatic duct links to the common bile duct.
Imaging tests can’t find pancreatic cancers that are still in their early stages. Because of this, a lot of people don’t find out they have cancer until it has spread (metastasis). Also, many popular cancer drugs don’t work on pancreatic cancer, which makes it extremely hard to treat.
What Are the Types of Pancreatic Tumors?

Among the diverse array of pancreatic tumors, two primary types take center stage—exocrine tumors and neuroendocrine tumors (NETs).
Exocrine Tumors
Exocrine tumors command the majority, constituting over 90% of all pancreatic tumors. The most prevalent in Exocrine tumors is adenocarcinoma, originating in the cells lining the organs.
Neuroendocrine Tumors (NETs)
Neuroendocrine tumors, accounting for less than 10% of pancreatic tumors, offer a unique perspective. Also known as Islet Cell Carcinomas, NETs introduce a different set of considerations in the context of pancreatic cancer.
Pancreatic cancer consists primarily of adenocarcinomas, which account for approximately 85% of the cases. People diagnosed with adenocarcinomas face a challenging journey with significantly lower survival rates compared to those with pancreatic neuroendocrine cancer, according to the Indian Journal of Medical Science.
Getting an early assessment and a personalized treatment plan are the keys to better results.
What are the Symptoms of Pancreatic Cancer?
Detecting pancreatic cancer early is challenging as symptoms typically appear once the tumor affects other digestive organs.
Common symptoms include
a. Jaundice (yellowing of the skin):
This occurs when the liver fails to process bilirubin properly, leading to a yellowish tint in the skin and eyes.
b. Dark urine and light-colored stool:
Dark urine may indicate liver issues, while light-colored stool suggests problems with bile flow from the liver to the small intestine.
c. Upper abdominal and middle back pain:
Pain in these areas can result from the tumor pressing on nearby nerves or organs.
d. Fatigue and itchy skin:
Fatigue may stem from the body’s effort to combat the cancer, and itchy skin can result from the liver’s struggle to process waste.
e. Nausea, vomiting, gas, or bloating:
These symptoms may arise as the tumor affects the digestive process.
f. Lack of appetite, blood clots, and weight loss:
The cancer’s impact on the digestive system can lead to reduced appetite and weight loss, and blood clots may occur due to changes in blood flow.
g. New-onset diabetes:
The development of diabetes may indicate pancreatic dysfunction, often linked to pancreatic cancer.
h. Pancreatitis (inflammation in the pancreas):
Inflammation in the pancreas is painful. This may be a sign of pancreatic cancer.
Symptoms for pancreatic neuroendocrine cancer may differ, including diarrhea and anemia.
i. Diarrhea:
An irregularity in bowel movements can be a symptom of neuroendocrine pancreatic cancer.
j. Anemia:
Lower-than-normal red blood cell levels can lead to fatigue and weakness, indicating a potential issue with pancreatic neuroendocrine cancer.
If you’ve recently developed diabetes or pancreatitis, your healthcare provider may suspect pancreatic cancer.
What are the Risk factors associated with Pancreatic Cancer?

While the exact causes of pancreatic cancer remain unavailable. There are various risk factors recognized as potential contributors to its development.
According to the National Library of Medicine, numerous risk factors play a role in the development of pancreatic cancer.
Let’s explore these risk factors that might increase the likelihood of pancreatic cancer:
1. Dietary Habits and High-Fat Content:
Intake of food rich in high-fat content is linked to elevated cholesterol levels, adversely affecting organ functionality, including the pancreas.
The damaged functionality may contribute to the development of pancreatic cancer.
2. Diabetes and Blood Sugar Levels:
Uncontrolled blood sugar levels are a characteristic of diabetes. They can disrupt the proper functioning of internal organs and cause severe damage.
This disruption creates an environment conducive to the development of pancreatic cancer.
3. Smoking and Cancer Cell Production:
Smoking is another primary cause of various cancers. It escalates the production of cancer cells while simultaneously harming healthy cells.
This heightened production of cancer cells increases the risk of pancreatic cancer.
4. Obesity, and Hormonal Imbalance:
Lack of exercise and obesity creates a fertile ground for hormonal imbalance. This is a significant risk factor for pancreatic cancer.
Regular physical activity, lasting at least 30 minutes daily, can help to fortify the immune system against various diseases.
5. Alcohol Consumption and Organ Functionality:
Excessive alcohol intake weakens the functionality of internal organs, including the pancreas.
This diluted functionality contributes to the vulnerability of developing pancreatic cancer.
6. Exposure to Toxic Chemicals:
Frequent exposure to toxic chemicals and pesticides without proper safety measures poses a risk factor for pancreatic cancer.
Adhering to required safety measures is crucial to reduce this risk.
7. Liver Damage and Pancreatic Cancer:
Prolonged kidney illness leading to liver damage enhances the exposure to pancreatic cancer.
The intricate relationship between the liver and pancreas in the digestive process plays a role in the development of this cancer.
8. Family History and Genetic Mutation:
A family history of pancreatic cancer among immediate family members or ancestors heightens the individual’s risk.
Genetic mutations within the family may contribute to the increased likelihood of developing pancreatic cancer.
Understanding and recognizing these risk factors is crucial for preventive measures and early detection.
How is pancreatic cancer diagnosed?

Detecting pancreatic cancer early poses a challenge as routine exams can’t feel the pancreas, and tumors are often elusive on standard imaging tests.
1. Pancreas Function Tests:
When pancreatic cancer is suspected, your healthcare provider may recommend a combination of tests, including
2. Imaging Tests:
Below is the list of imaging tests that should be performed:
a. CT (Computed Tomography) Scans:
CT scans utilize X-rays and computer technology to create detailed cross-sectional images of the pancreas This aids in the detection of abnormalities or tumors.
b. MRI (Magnetic Resonance Imaging):
MRI employs magnetic fields and radio waves to generate detailed images of the pancreas.
MRI provides valuable insights into its structure and identifying potential cancerous growths.
c. PET (Positron Emission Tomography):
PET scans involve a small amount of radioactive material to highlight areas with high metabolic activity.
This test helps to identify cancerous cells and their locations within the pancreas.
d. Endoscopic Ultrasound (EUS):
Endoscopic ultrasound combines endoscopy and ultrasound to obtain detailed images of the pancreas.
The EUS allows the visualization of tumors and provides information for diagnosis and treatment planning.
3. Blood Tests:
A pancreas blood test detects tumor markers, with elevated levels of carbohydrate antigen (CA) 19-9 indicating pancreatic cancer.
4. Staging Laparoscopy:
Providers may use laparoscopy to assess the extent of cancer and its removability. This minimally invasive procedure includes a camera-equipped tube inserted through small incisions.
5. Genetic Testing:
Upon a pancreatic cancer diagnosis, genetic testing is advised. It identifies hereditary factors and guides effective treatment.
Mutations in BRCA1 and BRCA2 genes, known for breast cancer, can indicate pancreatic cancer risk.
First-degree relatives should consider genetic testing to understand their risk, though having the mutation doesn’t guarantee cancer development. Understanding the risk aids in informed decision-making.
Have you ever wondered what happens inside the body when a person has pancreatic cancer? With this, we come to the next segment of complications of pancreatic cancer. Well, let’s break it down.
What are the complications of pancreatic cancer?
Pancreatic cancer tends to move or spread, a process called metastasis.
It starts by going to nearby blood vessels and lymph nodes. From there, it can travel to various organs like the liver and the lining of your abdominal cavity (known as the peritoneum), and even make its way to the lungs.
A lot of the time, pancreatic cancer has already spread beyond the pancreas by the time it is diagnosed.
Early detection and understanding of the complications can make a significant difference.
Resectable vs. Unresectable Pancreatic Cancer: What Sets Them Apart?

Healthcare providers categorize pancreatic tumors into four groups for effective diagnosis and treatment:
Resectable:
The tumor is confined to the pancreas without involving nearby blood vessels or organs.
Surgery is a viable option for complete removal.
Borderline Resectable:
The tumor is within the pancreas with some involvement of nearby blood vessels.
Although challenging, surgical removal is still possible.
Locally Advanced:
The tumor is in the pancreas with significant involvement of nearby blood vessels.
Surgical removal becomes difficult or unsafe in these cases.
Metastatic:
Cancer has spread to distant areas in the body, like the liver, lungs, or abdominal cavity.
Possible spread to nearby organs, tissues, or lymph nodes near the pancreas.
For more specific information about pancreatic cancer staging, consult your healthcare provider. Understanding your diagnosis empowers you to make informed decisions about your treatment.
How do doctors find the right treatment for pancreatic cancer?
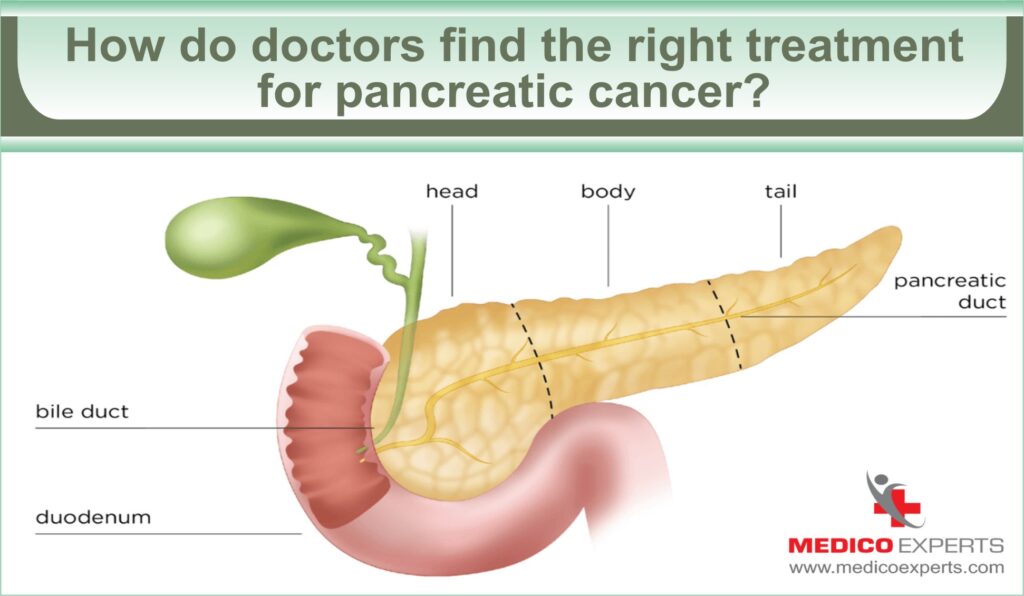
The treatment approach for pancreatic cancer is tailored based on specific factors:
Tumor Location:
Treatment varies depending on where the tumor gets located in the pancreas.
Cancer Stage:
The stage of cancer. This indicates the extent of the cancer spread and influences the chosen treatment.
Overall Health:
People’s health plays a role in determining the most suitable treatment plan.
The extent of Spread:
Whether the cancer has spread beyond the pancreas influences treatment decisions.
What Are the Stages of Pancreatic Cancer?
The TNM (Tumor, Nodes, Metastasis) staging system, developed by the American Joint Committee on Cancer, employs a combination of numbers and letters, such as stage 0 or stage 1A, to characterize the size and location of pancreatic cancer.
It is important to note that this system is seldom used for staging pancreatic cancer, typically only in cases where the patient does not undergo surgery.
This staging system takes into account:
T (tumor) size and whether the cancer has infiltrated blood vessels near the pancreas.
N (nodes), which denotes whether the cancer has spread to nearby lymph nodes.
M (metastasis), is determined by whether the cancer has disseminated to distant lymph nodes or organs.
Here’s a breakdown of the stages and their corresponding TNM indications for a more comprehensive understanding.
Stage 0 (carcinoma in situ):
The pancreas exhibits abnormal cells that have the potential to develop into cancer and extend to adjacent tissues.
Stage 1 pancreatic cancer (T1, N0, M0/T2, N0, M0):
The cancer is confined to the pancreas. Stage 1A refers to a tumor of 2 cm (0.8 inches) or smaller, while Stage 1B indicates a tumor ranging from 2 to 4 cm.
Stage 2 pancreatic cancer (T3 and N1, M0 or T3, N0, M0/T1, T2):
Stage 2A signifies a tumor larger than 4 cm. In contrast, Stage 2B describes a tumor of any size and cancer that has spread to one to three nearby lymph nodes.
Stage 3 pancreatic cancer (T1, T2, or T3, N2, M0/T4, any N, M0):
The cancer at this stage has spread to four or more lymph nodes near the tumor and/or major blood vessels near the pancreas, regardless of the tumor size.
Stage 4 pancreatic cancer (any T, any N, M1):
The tumor has metastasized to other parts of the body, such as the liver, lungs, or bones. In Stage 4, the tumor can be any size.
Now that we know where pancreatic cancer goes, how do we deal with it?
What are the Treatment Options for Pancreatic Cancer?
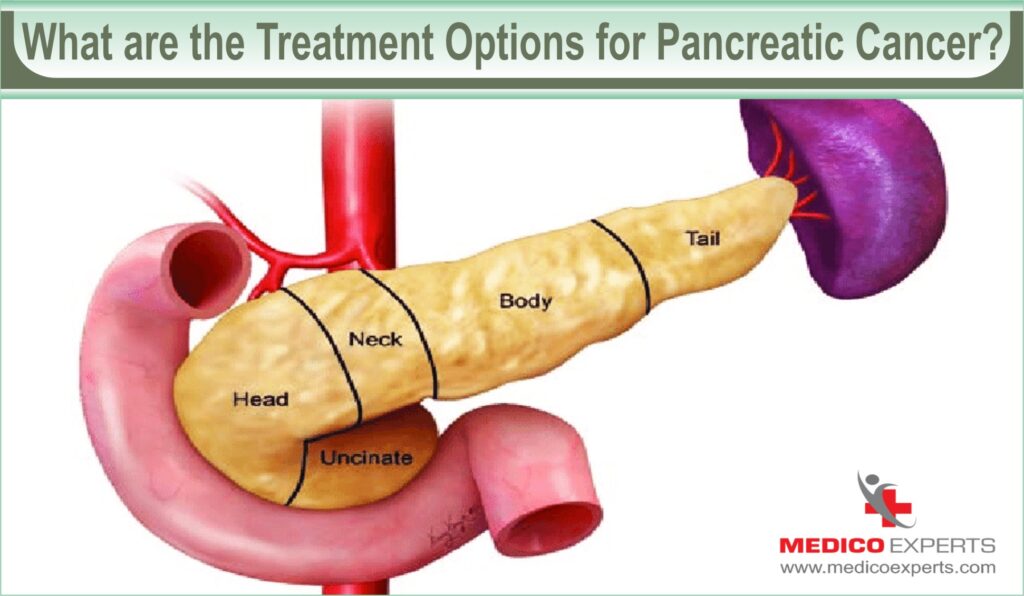
Treatment for pancreatic cancer involves a combination of approaches, and it depends on factors like the stage of cancer, the patient’s health, and the location of the tumor.
Here are some common treatment options:
1. Surgery:
Pancreatic cancer treatments primarily involve surgery. This is recognized as the most realistic way to achieve a cure. However, surgeons consider this option only if they believe complete removal of the cancer is feasible.
Several surgical techniques are available, contingent on the tumor’s location and size as mentioned earlier.
Some of the surgeries are as follows:
a. Whipple Procedure (Pancreaticoduodenectomy):
In cases where the tumor is in the head of the pancreas (the widest part, near the small intestine), the Whipple procedure may be recommended.
This surgical approach entails removing the pancreas’s head, the duodenum (first portion of the small intestine), the gallbladder, a section of the bile duct, and nearby lymph nodes.
Following the removal, the surgeon reconnects the remaining bile duct and pancreas to the small intestine. This helps to reestablish the digestive tract.
b. Distal Pancreatectomy:
If the tumor is in the tail of the pancreas, a distal pancreatectomy may be performed.
This involves removing the tail and part of the body of the pancreas. In most cases, the spleen (A compact organ situated beneath the left rib cage, slightly above the stomach.) is also removed.
Since the spleen aids in fighting infections, your healthcare provider might recommend certain vaccinations before the procedure.
c. Total Pancreatectomy:
In cases where cancer has spread throughout the entire pancreas, a total pancreatectomy may be considered if resection is still possible.
This surgery involves removing the entire pancreas, gallbladder, spleen, and parts of the stomach and small intestine.
Living without a pancreas comes with significant consequences. The pancreas produces insulin and other hormones crucial for regulating blood sugar.
Without it, diabetes develops, requiring insulin shots for survival. Additionally, digestive support is needed with pancreatic enzyme pills.
2. Chemotherapy:
Chemotherapy utilizes drugs designed to eliminate cancer cells.
It’s aided either in pill form or through an IV in your arm. It serves as a standalone treatment, especially for advanced pancreatic cancer.
Chemotherapy can be recommended before surgery to shrink tumors or after surgery to eradicate any remaining cancer cells.
3. Radiation Therapy:
High-energy X-rays are used in radiation therapy to kill cancer cells.
It’s commonly used in treating pancreatic cancer. Radiation therapy often combines it with chemotherapy (chemoradiation), recommending it before or after surgery, or as a primary cancer treatment.
Radiation therapy helps alleviate symptoms in advanced cases where surgery isn’t an option.
4. Targeted Therapy:
Targeted therapy involves drugs that specifically target certain proteins controlling cancer cell growth.
Doctors or health experts may combine targeted therapy with treatments like radiation therapy.
Common drugs for pancreatic cancer include Erlotinib, Olaparib, Larotrectinib, and Entrectinib.
5. Pain Management:
Pancreatic cancer can be intensely painful, involving nearby nerves.
Healthcare providers offer pain management through oral medications, anesthesia, or steroid injections.
If severe and persistent pain develops, inform your healthcare provider for tailored symptom relief.
How is Pancreatic Cancer Prevented?

While pancreatic cancer can’t be entirely prevented, certain steps can lower your risk:
1. Don’t smoke:
Avoiding tobacco significantly reduces your risk of pancreatic cancer.
2. Limit alcohol intake:
Moderating alcohol consumption contributes to a healthier lifestyle.
3. Eat a healthy diet:
Focus on fresh fruits, vegetables, and whole grains while reducing red meat, sugary drinks, and processed foods.
4. Avoid harmful chemicals:
Limit exposure to substances like asbestos, pesticides, and petrochemicals.
5. Maintain a healthy weight:
Strive for a weight that’s optimal for your health.
6. Pancreatic Cancer Screenings:
Routine screenings for pancreatic cancer aren’t typical, but for those with a higher risk due to genetic factors, healthcare providers recommend monitoring through imaging tests and endoscopic ultrasounds.
What is the pancreatic cancer treatment cost in India?

The expense of pancreatic cancer treatment in India is considerably more affordable than in highly developed nations.
The cost of pancreatic cancer treatment in India varies, ranging from INR 5,25,000 to INR 7,35,000 (USD 6728–USD 9420).
Despite the financial challenges associated with cancer care, India stands as a medical equivalent to leading global nations, providing top-notch treatment for all patients.
In our exploration of the topic is Pancreas Cancer Treatable? let’s conclude our blog post.
Takeaway
Recognizing the importance of early detection and awareness is crucial for improving outcomes in pancreatic cancer.
While screening a large population may not be practical. Trying to focus on high-risk groups, such as those with a family history, allows for targeted early detection efforts. Understanding risk factors is vital for effective prevention strategies.
In countries with limited resources and a lower Human Development Index (HDI), challenges in health infrastructure and diagnostic tools can impact outcomes in terms of incidence and mortality.
Prioritizing prevention and lifestyle changes becomes key to enhancing outcomes for pancreatic cancer patients, positively influencing prognosis and survival.
Consider reaching out to the expertise of the MedicoExperts Tumor Board, a specialized team ready to offer comprehensive guidance and tailored support for your unique situation.
The advantages of connecting with the team of MedicoExperts Tumor Board are as follows:
- Access a team with specialized knowledge in pancreatic cancer to make informed decisions.
- Receive guidance tailored to the specifics of your diagnosis and treatment plan.
- Benefit from an approach that considers both medical and emotional aspects of your journey.
- Connect with a network of professionals collaborating to ensure the best possible outcomes.
Remember, seeking guidance from the MedicoExperts Tumor Board can significantly enhance your understanding and management of pancreatic cancer. Schedule an appointment today and take the first step towards prioritizing your health.
FAQ’s :
Q1. How long can you live with pancreatic cancer?
A. Survival rates vary, but overall, pancreatic cancer has a low five-year survival rate, often due to late-stage diagnosis.
Q2. Can you live without a pancreas?
A. Yes, but it requires lifelong management, including insulin and digestive enzyme replacement. Seeking the expertise of the MedicoExperts Tumor Board can help to gain comprehensive support for navigating life without a pancreas.
Q3. Can pancreatic cancer be completely cured with treatment?
A: Complete cure depends on various factors, including the stage of cancer and the response to treatment. Early detection improves the chances of successful treatment.
Q4: Are there side effects of chemotherapy for pancreatic cancer?
A: Yes, chemotherapy can have side effects like nausea, fatigue, and hair loss. However, its goal is to target and kill cancer cells.
Q5. How does targeted therapy differ from chemotherapy?
A. Targeted therapy specifically targets abnormalities in cancer cells, while chemotherapy affects rapidly dividing cells, including both cancerous and healthy ones.



